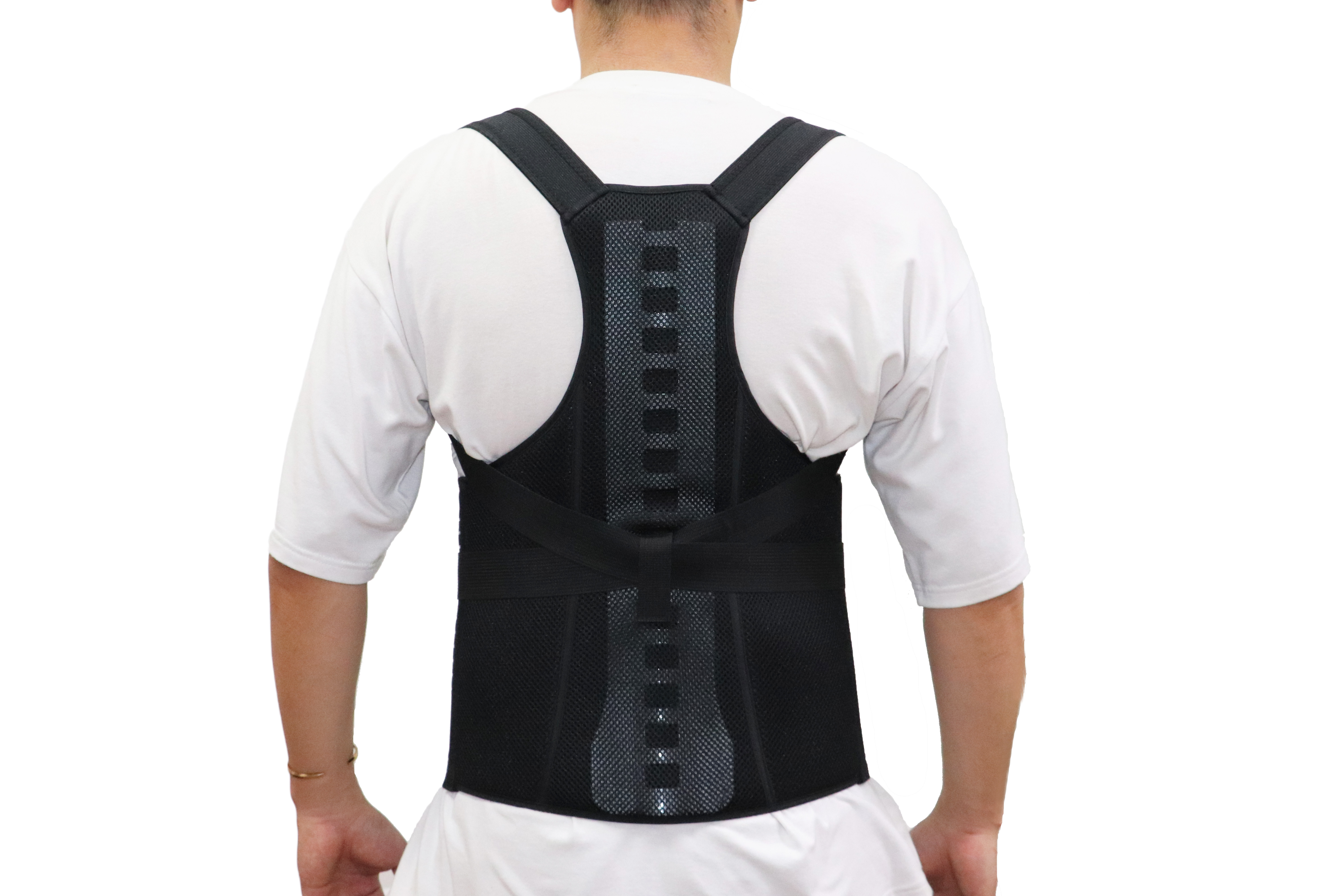
When and Why a Post-Surgery Back Stabilization Brace Is Clinically Indicated
Surgical Contexts Requiring Rigid Immobilization (e.g., Spinal Fusion, Laminectomy, Vertebroplasty)
Spinal fusion procedures, laminectomies, and vertebroplasties generally need some form of rigid support outside the body to keep the healing tissues and any implanted hardware safe. After surgery, wearing a back brace helps restrict movement between the vertebrae during important recovery periods like when bone grafts are integrating in fusion cases or when cement from vertebroplasty is setting up properly. This restriction actually cuts down on problems like hardware shifting or fractures happening at nearby segments of the spine. Research published in the Spine Journal last year found that patients who wore braces had about a 30% lower chance of experiencing these adjacent level fractures after vertebroplasty treatments. Most surgeons will recommend these stiff braces for their patients under certain conditions including...
- Multi-level instrumentation necessitates load redistribution across unstable segments;
- Osteoporosis or compromised bone quality threatens bony integrity;
- Early patient mobility exceeds biomechanically safe thresholds.
Timeline Guidelines: Acute vs. Subacute Phases and Duration of Brace Use
Bracing protocols align with biologically driven recovery phases. During the acute phase (0–6 weeks), continuous wear is standard to maximize immobilization and safeguard tissue healing. In the subacute phase (6–12 weeks), structured weaning begins:
- Reduce daily wear time by 2-hour increments each week;
- Discontinue use during low-risk seated activities (e.g., meals, physical therapy);
- Maintain bracing during ambulation or prolonged standing until cleared.
The 2023 Spinal Recovery Consensus suggests patients wear braces full time for about 8 to 10 weeks following complex spinal fusions. But this isn't one size fits all really. Things like how dense someone's bones are, how complicated their surgery was, and whether they actually follow through with wearing the brace make a big difference in recovery results. A study found that roughly 23 percent of people stop wearing their braces too soon because it just plain hurts too much according to the Journal of Orthopaedic Surgery. This shows why getting comfortable with the brace early on matters so much, along with proper education about what to expect during recovery.
Matching Brace Type to Anatomy and Surgical Goal: Thoracolumbar, Lumbar, and Custom Solutions
Selecting the optimal post-surgery back stabilization brace hinges on precise alignment between anatomical coverage, surgical objective, and biomechanical demand. Mismatched bracing increases reoperation risk by 18%, per a 2023 analysis in the Journal of Spinal Disorders—a strong signal that “one-size-fits-all” approaches compromise safety and efficacy.
Thoracolumbar Orthoses (TLSO) for Multi-Level Stabilization After Fusion or Trauma
TLSO braces provide rigid support around the entire torso area, extending from the lower part of the back down to the pelvis region. Because of this comprehensive stabilization, they're often considered the best option when dealing with complex spinal issues like multiple level fusions, serious fractures, or surgical revisions. The way these braces are constructed helps take pressure off the implanted hardware. Studies suggest that TLSO support can cut down mechanical stress on screws and rods by about 30 to maybe even 40 percent compared to regular soft supports according to Biomechanics Research in 2023. This kind of stress management actually promotes better bone healing while also protecting the metal components from wearing out too quickly.
Lumbar Supports vs. Hybrid Designs for Selective Load Sharing in Minimally Invasive Procedures
When dealing with less complex procedures like microdiscectomies or single level TLIF surgeries, lumbar supports and hybrid back braces actually work pretty well for most patients. The cool thing about these braces is they can be adjusted to limit forward and backward movement but still allow some side to side motion and twisting. This kind of partial support helps keep the muscles active rather than completely shutting them down, which tends to speed up recovery time. Some recent research from 2022 showed interesting results too. People who wore these adjustable hybrid braces got back to doing their daily activities on their own about 15 days faster compared to folks stuck in those old school rigid TLSO braces. Makes sense really since allowing limited movement probably keeps blood flowing better and prevents muscle atrophy during recovery.
Evidence, Controversy, and Practical Trade-Offs in Post-Surgery Back Stabilization Brace Use
While bracing remains routine in many practices, its clinical value is neither uniform nor universally supported. Evidence reveals meaningful gaps in pain relief, fusion success, and long-term function—prompting growing scrutiny over indications, duration, and alternatives.
What the Literature Says: Efficacy Gaps in Pain Reduction, Fusion Rates, and Long-Term Function
Looking at all the research together, bracing doesn't seem to make much difference in short term pain relief either. Patients wearing braces typically see around a 1.5 point improvement on the Visual Analog Scale compared to just 1.2 points for those without them. We haven't actually seen any top notch randomized trials where bracing alone made a real statistical difference when it comes to how well bones fuse together after single level spinal procedures. And what about longer term outcomes? Studies following patients for two years find basically no difference in daily living abilities, walking patterns, or how people rate their own functioning whether they wore a brace or not. What this tells us is probably pretty straightforward really. How aggressively someone rehabilitates, what kind of education they receive about their condition, and getting moving sooner rather than later might matter far more for recovery than how long someone stays in a brace.
Adherence Challenges: Balancing Compliance, Comfort, and Clinical Necessity
Sustained brace use faces real-world barriers:
- Discomfort—rigid orthoses impair diaphragmatic excursion and increase skin shear, contributing to abandonment in up to 40% of users by week six;
- Deconditioning risk—prolonged immobilization accelerates paraspinal atrophy, potentially undermining long-term stability;
- Functional disruption—challenges with sleeping, driving, and personal care reduce practical utility and erode motivation.
Evidence-based weaning—initiated alongside physical therapy at week 4–6—improves adherence without compromising outcomes. Ultimately, the decision to prescribe, continue, or taper bracing must reflect not just surgical anatomy, but also patient physiology, goals, and lived experience.
FAQ
What are the main types of post-surgery back braces?
The main types are Thoracolumbar Orthoses (TLSO) for larger stabilizations, lumbar supports for more focused areas, and hybrid designs for selective load sharing in minimally invasive procedures.
How long should one wear a back brace after surgery?
It varies by individual circumstances, but generally full-time wear is recommended for about 8 to 10 weeks following complex procedures, with gradual weaning as healing progresses.
Do post-surgery back braces aid in pain relief?
Braces may provide some pain relief, but studies indicate they do not significantly improve outcomes in long-term pain reduction or functional recovery.
Why might patients stop wearing their braces prematurely?
Discomfort, the risk of deconditioning, and disruptions to daily activities such as sleeping and driving can lead patients to stop wearing braces earlier than advised.